Surgeons from the University of Alberta's Office of Global Surgery are helping address the worldwide shortage of life-saving ventilators during the COVID-19 pandemic.
And they are warning that the push to ration existing equipment and scale up production of new equipment could lead to unfair, harmful and even deadly consequences.
"The world needs to co-ordinate the quality, cost, manufacturing capacity and equitable distribution of ventilators," said Abdullah Saleh, a pediatric surgeon at Edmonton's Stollery Children's Hospital who heads the Office of Global Surgery.
Saleh and nine doctors, ethicists and health economists from Alberta, British Columbia and the United States have written a white paper outlining guiding principles for the response to the global ventilator shortage.
The paper has been shared with Health Canada and medical device industry executives, among others, through the advocacy group Safe Affordable Ventilators for All (SAVA).
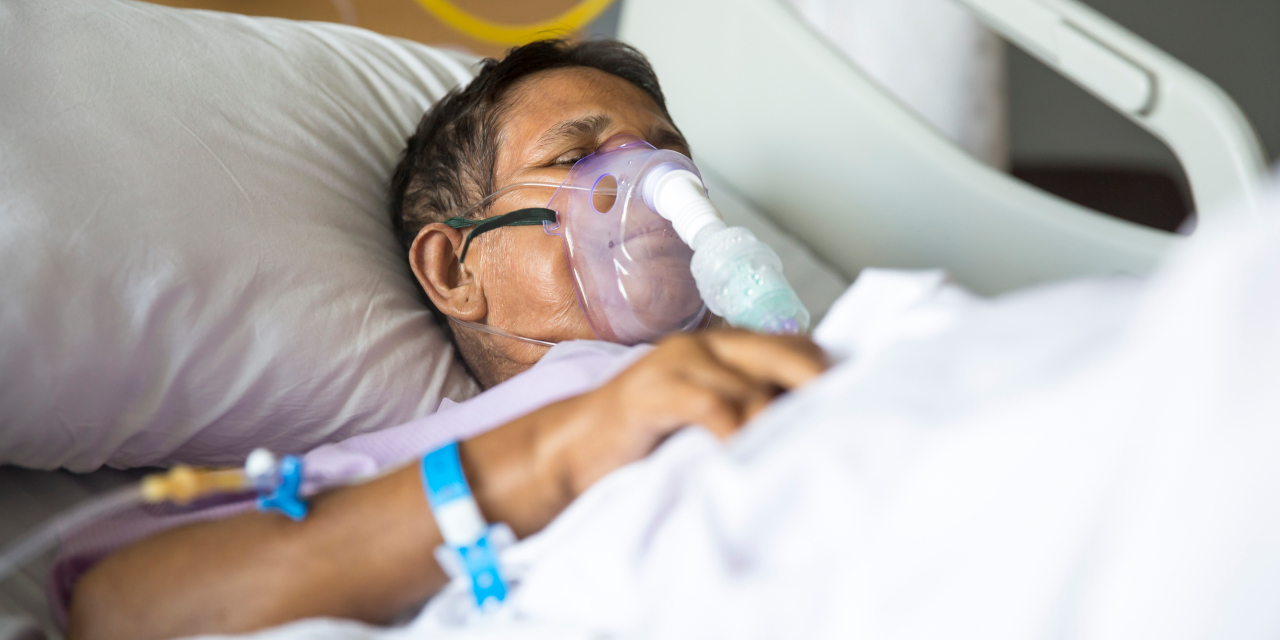
Ventilators are critical life-saving equipment in the COVID-19 pandemic because they mechanically pump oxygen into a patient's lungs when their ability to breathe on their own fails.
The group estimates that five to 10 per cent of COVID-19 patients will get sick enough to require ventilation, and the deficit of ventilator units in the United States could be as high as 75,000 units and more than 800,000 globally.
Engineers, designers and health-care professionals around the world are collaborating to build and distribute the complex life-support technologies. Saleh said these efforts are commendable, but noted the risk of distributing poor-quality and unreliable ventilators is almost as dangerous as the risk posed by the lack of ventilators.
"While it's very true that the need is urgent, it's important not to think that somebody can make a ventilator in their garage and put their grandfather on it-that was what we started to hear from this open-source community of engineers and developers," Saleh said. "This DIY, open-source, tech-focused approach can potentially cause problems.
"If you put someone on a ventilator that was not tested and it malfunctions, you may have a 100 per cent mortality for that patient."
A challenge to maintain standards, plan carefully under time pressure
Saleh has successfully worked on various not-for-profit projects to develop and produce low-cost water filters, high-efficiency stoves and electronic health records systems for lower-income countries in South America, East Africa and Southeast Asia through the not-for-profit Innovative Canadians for Change.
He said while it is tempting to jump in with immediate solutions, it is important to follow the basic medical principle to "do no harm."
"When there is high stress, high pressure and short timelines, the most important thing is to spend most of our time thinking about the ethics of the situation, and then act only once we've thought things through."
The Safe Ventilators team promotes a three-pronged approach to obtain adequate ventilating equipment for the worldwide need.
The first is to develop and widely distribute "Ambu bags," handheld devices often used by first responders for patients with milder symptoms who need breathing support. Some groups have looked at automating Ambu bags by adding a motor, but they have not passed regulatory requirements.
The second approach is to expedite development, testing and approval of simpler full-ventilator designs that can be produced for less than $1,000 each, while maintaining the highest safety standards. These would be very useful for health-care systems that lack the resources to purchase the expensive designs that are currently available.
The third strategy, which they believe is the safest and most effective for the short term, is to ramp up production of existing, highly complex, already approved ventilator models through existing production lines, but possibly also in facilities usually devoted to other manufacturing such as auto parts. The Government of Canada recently announced its plan to produce 30,000 additional ventilators using this third strategy.
Saleh said the fact that the highly contagious novel coronavirus affected higher-income countries in Europe and North America first may bring needed attention to the plight of lower-income countries, where ventilators are in even shorter supply.
He pointed out that ventilators are only part of the solution, and that a comprehensive approach to strengthening worldwide health-care capacity and planning for surge events such as the COVID-19 pandemic is critical.
"It seems like this is one of the first global events that has brought attention to the interconnectedness of the world and how fragile our health systems are," he said. "It highlights that we need to make these life-saving interventions available to the rest of the world.
"There is no protecting ourselves," he added. "We are vulnerable as long as the rest of the world is disadvantaged.
"There is only 'we' in this."