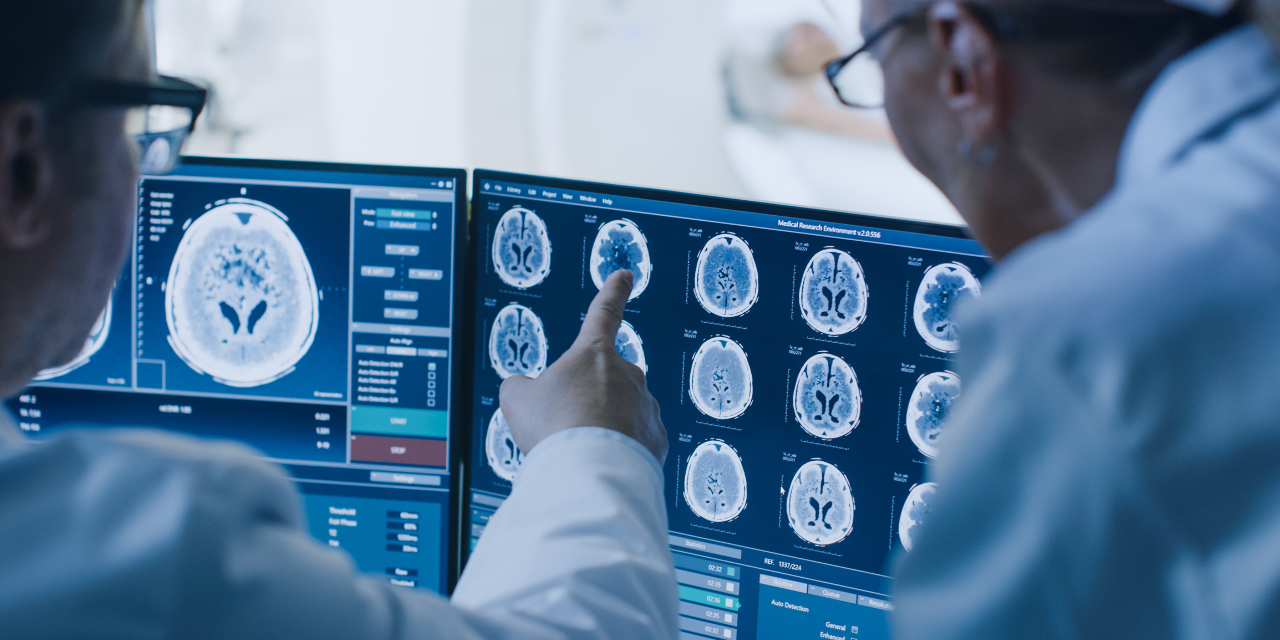
Neurologists at the University of Alberta are monitoring Edmonton patients diagnosed with COVID-19 for signs that the virus, which can cause deadly respiratory illness, may also attack the brain.
"Several manuscripts have been published that suggest patients with severe COVID-19 symptoms also display neurological problems such as confusion, stroke-like attacks, even a hemorrhage in the brain or less severe symptoms such as a loss of the sense of smell," said Christopher Power, professor of neurology and principal investigator of the Brain Power Lab.
"Many of the patients who have been found to have neurologic symptoms in the academic reports from Italy, China and the U.S. appear to be the sicker patients," said Jennifer McCombe, associate clinical professor of neurology, who is leading the initiative to look at patients locally.
Power and McCombe, who are both members of the Neuroscience and Mental Health Institute, normally treat patients with multiple sclerosis, HIV and brain infections. Neither is surprised that the novel coronavirus is attacking the brain-it is known that other coronaviruses have done so-but they said it is not common and the mechanism is not well understood.
"One major question that remains uncertain is to what extent does the virus gets into the brain to cause damage, or are the neurologic symptoms merely a consequence of the systemic effects of overactivation of the immune system?" said Power.
"Some viruses-and we're suspicious it is the case with COVID-19-infect the lining of the blood vessels and then use that as an entrance into the brain," he said.
"Other viruses like HIV actually use a Trojan horse strategy. They infect blood cells and then those blood cells transport the virus into the brain."
Power reported that approximately one per cent of patients with severe acute respiratory syndrome (SARS), caused by another coronavirus that broke out in 2003, also faced neurologic disabilities. They experienced stroke-like events, muscle weakness and peripheral nerve damage. The virus was later detected in brain tissue of some deceased SARS patients.
McCombe plans to examine electroencephalogram and MRI images of COVID-19 patients to understand their neurologic symptoms. A cerebral spinal fluid test has not yet been developed for COVID-19 but would also be very helpful as a window into the brain. Post-mortem analyses can be done to look for signs of the virus in the brain tissue and blood vessels.
McCombe said it is key to understand whether neurologic impairments are caused directly by the virus or whether they are secondary symptoms due to systemic inflammation.
"That will really help us decide on potential therapies that could prevent some of these neurologic problems," she said. "Do we need to focus on prevention therapies that relate to the issues that are happening elsewhere in the body, or is there viral invasion into the brain and therefore we need to continue to try to find therapies to treat the virus itself?"
If you think you have neurologic symptoms
Power said that anosmia, a loss of the senses of smell and taste, has presented in some otherwise asymptomatic COVID-19 patients. He said anyone who develops this symptom should monitor themselves for other symptoms such as a fever or cough.
McCombe said more dramatic changes in a person's cognitive functioning are a definite cause for concern, because there can be so many potential causes besides COVID-19.
"For an isolated change in smell, I would direct people to continue to maintain self-isolation measures," she said. "Someone exhibiting confusion or stroke-like symptoms should seek medical attention immediately."
Power said he is speaking daily with other members of the International Society for NeuroVirology so they can work together to track neurologic symptoms in COVID-19 patients.
"What we learn from COVID-19, we can apply to the next viral pandemic. The idea is to develop diagnostics and new treatments as soon as possible."